Review Article
Volume 2 Issue 2 - 2019
Beyond Glycemic Control: Cardiovascular Benefits with Empagliflozin and Linagliptin Combination.
1Dr. Sneha Thakur, Manager, Department of Medical Affairs, Lupin Ltd, Mumbai, India
2Dr. Bhavesh Lalan, Manager, Department of Medical Affairs, Lupin Ltd, Mumbai, India
3Dr. Amit Bhargava, VP and Head, Department of Medical Affairs, Lupin Ltd, Mumbai, India
2Dr. Bhavesh Lalan, Manager, Department of Medical Affairs, Lupin Ltd, Mumbai, India
3Dr. Amit Bhargava, VP and Head, Department of Medical Affairs, Lupin Ltd, Mumbai, India
*Corresponding Author: Sneha Thakur, Manager, Department of Medical Affairs, Lupin Ltd, India.
Received: November 27, 2018; Published: January 04, 2019
Abstract
Cardiovascular disease (CVD) is one of the most common macro vascular comorbidity in type 2 diabetes (T2DM). It has been reported that CVD is associated with as much as twice the number of deaths in T2DM patients. The current need is of a comprehensive approach to T2DM with concomitant CVD. Scientific literature recommends early use of combination therapy in T2DM patients with a high risk of CVD. Considering the published data on CV benefits with Empagliflozin and linagliptin, combination therapy with these two drugs may be useful in preventing and delaying the progression of CVD in T2DM patients. This review highlights the clinical evidence and the possible mechanisms for CV benefits with Empagliflozin and linagliptin.
Keywords: T2DM; CVD; Combination therapy; Empagliflozin; Linagliptin
Introduction
It is known that patients with type 2 diabetes mellitus (T2DM) have an increased risk for cardiovascular disease (CVD) (myocardial infarction, stroke, peripheral vascular disease), and CVD is the major cause of death in diabetics. [1] Studies always have proven that lowering HbA1c in T2DM patients has either no [2,3] or only a modest [4,5] effect on reducing cardiovascular (CV) risk. Contrary to this, managing traditional CVD risk factors like cholesterol and blood pressure, may markedly reduce CVD risk and related mortality in these patients. [1]
Scientific data from recently published trials such as LEADER (Liraglutide Effect and Action in Diabetes: Evaluation of Cardiovascular Outcome Results) [6] and SUSTAIN-6 (Trial to Evaluate Cardiovascular and Other Long-term Outcomes with Semaglutide in Subjects with Type 2Diabetes) [7] evidently prove that glucagon-like peptide 1 receptor agonists (GLP-1 RAs) (liraglutide and semaglutide) may reduce CVD risk along with their glucose-lowering effect and reduce other CVD risk factors in T2DM patients with pre-diagnosed CVD. Robust cardiovascular outcome studies like EMPA-REG OUTCOME (Empagliflozin Cardiovascular Outcome Event Trial in Type 2 Diabetes Mellitus Patients) [8], IRIS (Insulin Resistance Intervention After Stroke Trial) [9], and Proactive (Prospective pioglitazone Clinical Trial In macro vascular Events) [10] showed reduction in major adverse cardiac events (MACE) end points of 14%, 24%, and 16% (main secondary end point) respectively. The results from these studies highlight the fact that we are stepping into a new era in T2DM treatment, where the need to highlight the CV benefits of newer anti-diabetes medications, in addition to lowering plasma glucose is emphasized. It is important to demonstrate that the beneficial effects on the cardiovascular status is independent of reduction in PPG and FPG.
CVD mortality in T2DM patients
Table 1 represents the data regarding the rates of mortality associated with CVD in persons with T2DM.
Table 1 represents the data regarding the rates of mortality associated with CVD in persons with T2DM.
| Disease | Author (year) | Patients | n | CVD deaths | % Death rate | % CVD proportion of all deaths |
| CVD | Malik (2015) [12] | T2DM adults | 121,523 | 3722 | 3.10% | 21.10% |
| CVD | Salinero-Fort (2016) [13] | T2DM Adults | 2442 | 96 | 3.90% | 47.30% |
| CVD | Salinero-Fort (2016) [13] | T2DM adults + kidney disease | 965 | 124 | 12.80% | 56.10% |
| CAD | Carnethon (2010) [14] | T2DM only | 659 | 132 | 20% | 28.20% |
| CAD | Carnethon (2010) [14] | T2DM + CVD | 260 | 111 | 42.70% | 50.70% |
| CAD | Jackson (2012) [15] | Male diabetics | 116,145 | 6000 | 5.20% | 27.20% |
| CAD | Jackson (2012) [15] | Female diabetics | 100,507 | 4554 | 4.50% | 22.10% |
| CHF | Mazza (2007) [16] | Male diabetics | 202 | 22 | 10.90% | ------ |
| CHF | Mazza (2007) [16] | Female diabetics | 379 | 29 | 7.70% | ------ |
| MI | Shestakova (2016) [17] | T2DM adults | 3,060,516 | 3393 | 0.10% | 5.10% |
| SCD | Kucharska-Newton (2010) [18] | T2DM adults | 1550 | 69 | 4.50% | ---- |
| Stroke | Jackson (2012) [15] | Male diabetics | 116,145 | 1942 | 1.70% | 8.80% |
| Stroke | Jackson (2012) [15] | Female diabetics | 100,507 | 2436 | 2.40% | 11.80% |
Table 1: Prevalence of mortality associated with CVD in persons with T2DM [11].
CAD coronary artery disease (variously reported as coronary heart disease or ischemic heart disease), CBV cerebrovascular disease, CHF congestive heart failure (also reported simply as heart failure), CVD cardiovascular disease, MI myocardial infarction, NR not reported, SCD sudden cardiac death, T2DM type 2 diabetes mellitus. Weighted average of rates taken only for patients with T2DM and where complete outcomes were reported; thus, the number does not represent the sum of all of the numbers in the column above it.
Need to fill the treatment gap
As demonstrated in table 1, T2DM increases the propensity of CVD. The current need is to find a therapeutic measure which is not only fast acting but also provides sustained beneficial effects on glycemic control thereby delaying the onset and progression of CVD. [19] Current trends suggest the use of fixed dose combinations comprising of agents having complementary actions to reduce macrovascular complications. One such combination is empagliflozin and linagliptin. [19] Linagliptin is known to enhance levels of postprandial insulin and decrease glucagon secretion following food intake. [9,10] Also, linagliptin elevates insulin secretion and reduces glucagon secretion in a glucose-dependent manner, thereby reducing the probability of hyperglycemia with minimal risk of hypoglycemia. [19] Additionally, current literature suggests that it is weight neutral. [19]
As demonstrated in table 1, T2DM increases the propensity of CVD. The current need is to find a therapeutic measure which is not only fast acting but also provides sustained beneficial effects on glycemic control thereby delaying the onset and progression of CVD. [19] Current trends suggest the use of fixed dose combinations comprising of agents having complementary actions to reduce macrovascular complications. One such combination is empagliflozin and linagliptin. [19] Linagliptin is known to enhance levels of postprandial insulin and decrease glucagon secretion following food intake. [9,10] Also, linagliptin elevates insulin secretion and reduces glucagon secretion in a glucose-dependent manner, thereby reducing the probability of hyperglycemia with minimal risk of hypoglycemia. [19] Additionally, current literature suggests that it is weight neutral. [19]
Empagliflozin on the other hand works by inhibiting renal glucose reabsorption thereby promoting glucosuria, this effect is non-insulin dependent. The main pathological feature of T2DM is progressive and continuous deterioration of beta-cell function. However, treatment with empagliflozin increases the levels of plasma glucagon, which in turn is associated with an increase in endogeneous hepatic glucose production. [19] This further explains addition of linagliptin, that has an inhibitory effect on glucagon. This is thought to have the potential to decrease endogenous glucose production thereby improving the glucose-lowering capacity of empagliflozin. [19]
Scientific literature demonstrates that good and sustained glycemic control may delay the onset and progression of macrovascular complications including CVD. [20] Thus, combination treatment with linagliptin and empagliflozin appears to be a promising option in T2DM with concomitant macrovascular complications such as CVD.
Empagliflozin and Cardiovascular benefits
A reduction by 38%, 35%, 34% in CV mortality, HF hospitalization and a composite of CV mortality or HF hospitalization respectively was noted in T2DM patients with concomitant CVD in the EMPA-REG OUTCOME trial. These outcomes appeared identical in those with/without a pre-existing diagnosis of HF at the baseline. [8] These findings were in accordance with another analysis stating similar effects of empagliflozin on CV mortality and HF hospitalizations. [21] These analyses therefore further reinforce the recent ESC HF guideline, stating an important and indispensable role of empagliflozin in T2DM patients for preventing and delaying the onset of HF, thereby improving the life expectancy. [21]
A reduction by 38%, 35%, 34% in CV mortality, HF hospitalization and a composite of CV mortality or HF hospitalization respectively was noted in T2DM patients with concomitant CVD in the EMPA-REG OUTCOME trial. These outcomes appeared identical in those with/without a pre-existing diagnosis of HF at the baseline. [8] These findings were in accordance with another analysis stating similar effects of empagliflozin on CV mortality and HF hospitalizations. [21] These analyses therefore further reinforce the recent ESC HF guideline, stating an important and indispensable role of empagliflozin in T2DM patients for preventing and delaying the onset of HF, thereby improving the life expectancy. [21]
Figure 1 denotes the possible mechanisms through which empagliflozin demonstrates ‘cardio-protective’ benefits. It has been hypothesized that the cardio-protective benefits may be due to a shift in myocardial fuel metabolism away from energy inefficient glucose and fat towards an energy-efficient super fuel like ketone bodies, thereby improving myocardial function and efficiency. It has been postulated that even minute beneficial changes in energy mechanics may be responsible for larger improvements in myocardial work efficiency leading to substantial and sustained improvements in cardiac outcomes over weeks to months. [22]
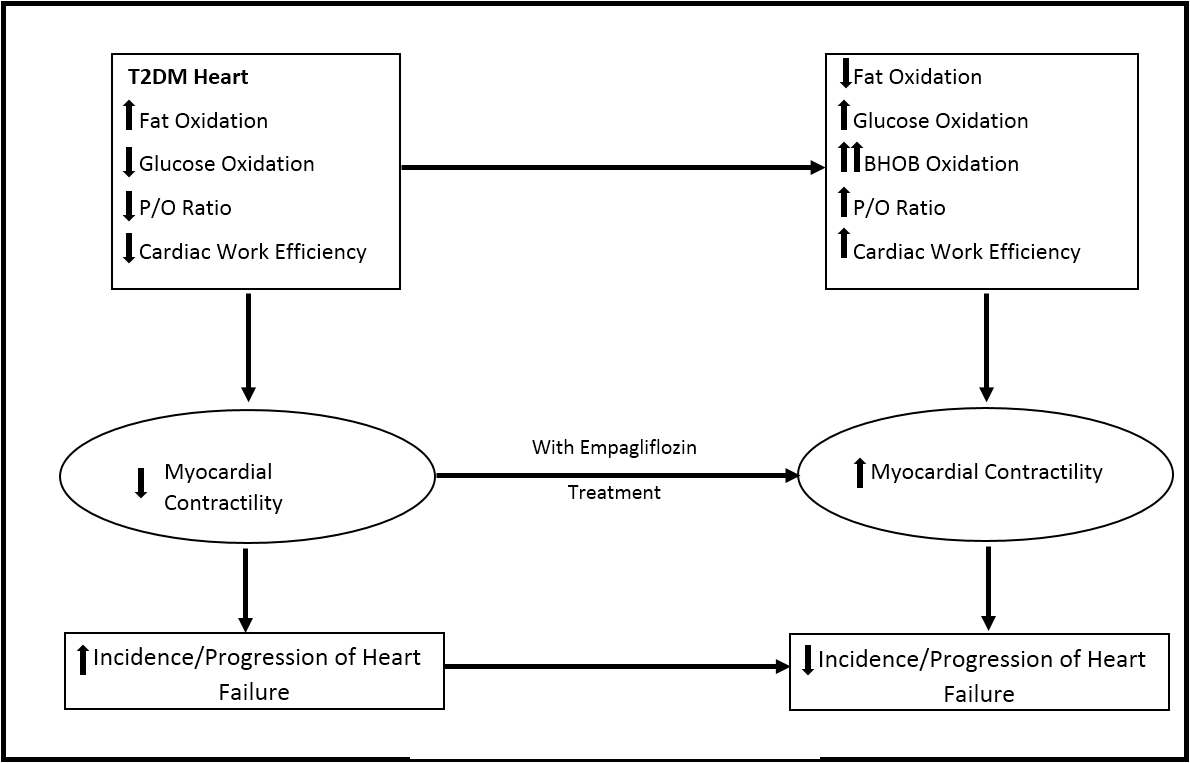
Figure 1: Myocardium fuel metabolism before and after empagliflozin therapy. [22]
P/O ratio indicates the number of ATP molecules produced per oxygen atom reduced by the mitochondrial electron transport chain.
P/O ratio indicates the number of ATP molecules produced per oxygen atom reduced by the mitochondrial electron transport chain.
In T2DM with concomitant HF, myocardial dysfunction results from impaired fatty acid oxidation and aberrant glucose uptake and oxidation. It is known that ketone bodies are a super fuel and act as a source of energy when there is restricted fuel selection and low energetic reserve thereby establishing a setting of more efficient ATP generation as compared to glucose and fatty acids. [22,23] An apparent metabolic advantage in failing diabetic heart is the ability to use ketones as a source of energy. Moreover, it has been observed that there is an increased level of ketone bodies in patients with HF and in patients on empagliflozin treatment. [22] Furthermore, the failing myocardium has an increased potential to effectively utilize ketone bodies as an alternative fuel resource. [22] A significant point here is that the remarkable CV outcomes observed in EMPA-REG OUTCOME study in patients with a history of pre-existing HF and in those without HF may be linked to the shift in fuel mechanism after empagliflozin treatment. Along with an improvement in fuel metabolism, neurohormonal/vascular effects, BP reduction, natriuretic and diuretic effects may be responsible for such outcomes with empagliflozin but their potential to produce beneficial results within 3 months is dubious. [22] In light of these findings and hypothesis of fuel shift mechanism, empagliflozin may be regarded as a ‘Cardio-protective’ drug.
Linagliptin and CV benefits
It was demonstrated in a CV meta-analysis that linagliptin may either have a beneficial or a neutral effect on CV outcomes in a significant number of patients with T2DM compared with control treatments. Furthermore, the risk for CV events was unchanged, or lowered, across several pre-specified subgroups based on key demographic and clinical characteristics. These results include comparisons with placebo, as well as two active comparators, namely glimepiride and voglibose, either as monotherapy or in combination with common oral glucose-lowering drugs. [24]
It was demonstrated in a CV meta-analysis that linagliptin may either have a beneficial or a neutral effect on CV outcomes in a significant number of patients with T2DM compared with control treatments. Furthermore, the risk for CV events was unchanged, or lowered, across several pre-specified subgroups based on key demographic and clinical characteristics. These results include comparisons with placebo, as well as two active comparators, namely glimepiride and voglibose, either as monotherapy or in combination with common oral glucose-lowering drugs. [24]
Furthermore, a comprehensive pooled analysis assessed patient level data from around 9450 diabetic subjects who participated in 19 clinical trials. This analysis represents approximately twice the exposure to linagliptin in terms of patient years as compared to previous analyses. The results of this new analysis suggest that linagliptin does not increase the risk of CVD compared with the comparator or placebo which is in agreement with the previous analysis. Another interesting observation in this study was that the incidence of CV events with linagliptin was only 13.4 per 1000 patients and 18.9 for other comparators. [25]
According to the recently published CARMELINA trial, linagliptin when added to usual care in adult T2DM patients demonstrated non-inferiority for the risk of composite CV outcome for a median period of 2.2 years. [26] This result is in agreement with the previous meta-analysis. However, there was no statistically significant difference between linagliptin and placebo groups in the risk of hospitalization for heart failure. The relevance of this finding is particularly in relation to earlier reports with Saxagliptin (SAVOR-TIMI 53) [27] and alogliptin (EXAMINE) [28] that documented statistically significant and numerical increase in hospitalization for heart failure; whereas sitagliptin (TECOS) [29] demonstrated a neutral effect.
Several mechanisms may be responsible for the impressive CV benefits with linagliptin. Most importantly, linagliptin has demonstrated significant and sustained reductions in PPG thereby reducing glycemic variability without potential adverse effects like hypoglycemia and weight gain. [24,30] Another possible mechanism could be increase in incretin hormone levels that may provide beneficial cardio-protection as experimental data suggest that elevated GLP-1 levels positively regulate lipid metabolism [24,30], reduce infarct size and recuperate cardiac function. [30] However, further research is warranted in this regard. It has also been studied experimentally that DPP-4 substrates not only comprise of incretins but also of vasoactive peptides that play a major role in inflammation, immunity, and CV function; evidence from preclinical studies show that reduced DPP-4 activity can minimize inflammation, hasten endothelial repair, thereby reducing ischemic injury. [24,31] Finally, linagliptin’s xanthine-based molecular structure confers inherent anti-oxidative properties. [24] It is because of these properties linagliptin both directly through reducing reactive oxygen species and indirectly through mediating inflammatory markers along with hastening of endothelial repair is thought to reduce atherosclerotic burden. [32] Because of these attributes linagliptin may be considered as a ‘Cardio-safe’ drug.
CV benefits with the Combination
Current evidence suggests that both empagliflozin and linagliptin have favorable cardiovascular data. Additionally, it has been reported that the combination treatment with empagliflozin and linagliptin in drug naïve patients, [33] where metformin therapy failed [34] and in patients where intensive glycemic control is indicated that cannot be achieved with dual therapy of metformin and empagliflozin or linagliptin [35,36] is efficacious and demonstrated significant reductions in HbA1c and FPG. Furthermore, treatment with this combination showed added benefit of BP and weight reduction which are established CVD risk factors. Also, the glycemic control with this combination was sustained for a period of 52 weeks indicating lesser chance of glycemic variability. [34-37] This may further support the CV safety of this combination.
Current evidence suggests that both empagliflozin and linagliptin have favorable cardiovascular data. Additionally, it has been reported that the combination treatment with empagliflozin and linagliptin in drug naïve patients, [33] where metformin therapy failed [34] and in patients where intensive glycemic control is indicated that cannot be achieved with dual therapy of metformin and empagliflozin or linagliptin [35,36] is efficacious and demonstrated significant reductions in HbA1c and FPG. Furthermore, treatment with this combination showed added benefit of BP and weight reduction which are established CVD risk factors. Also, the glycemic control with this combination was sustained for a period of 52 weeks indicating lesser chance of glycemic variability. [34-37] This may further support the CV safety of this combination.
In summary, combination of empagliflozin and linagliptin has the potential to exert benefits beyond lowering glucose, such as improvement in fuel metabolism, neurohormonal/vascular effects, BP reduction, weight reduction, natriuretic and diuretic effects, this combination may be regarded as ‘cardio-therapeutic’ as it may improve the heart health in a diabetic patient. In light of these evidences, this combination may be regarded as one the promising options in T2DM management with associated risk or pre-existing CVD. However, further research in this regard is warranted.
Acknowledgement
Nil
Nil
Conflict of Interest
Authors are employees of Lupin Ltd.
Authors are employees of Lupin Ltd.
References
- Abdul-Ghani M., et al. “Cardiovascular Disease and Type 2 Diabetes: Has the Dawn of a New Era Arrived?” Diabetes Care 40.7 (2017): 813–820.
- Action to Control Cardiovascular Risk in Diabetes Study Group. Effects of intensive glucose lowering in type 2 diabetes. N Engl J Med358.24 (2008): 2545–2559.
- ADVANCE Collaborative Group. “Intensive blood glucose control and vascular outcomes in patients with type 2 diabetes”. N Engl J Med358.24 (2008): 2560-72.
- Duckworth W., et al. “Glucose control and vascular complications in veterans with type 2 diabetes”. N Engl J Med 360.2 (2009): 129-39.
- UK Prospective Diabetes Study (UKPDS) Group. “Intensive blood-glucose control with sulphonylureas or insulin compared with conventional treatment and risk of complications in patients with type 2 diabetes (UKPDS 33)”. The Lancet 352.9131 (1998): 837-53.
- Marso SP., et al. “Liraglutide and cardiovascular outcomes in type 2 diabetes”. N Engl J Med 375.4 (2016): 311-22.
- Marso SP., et al. “Semaglutide and cardiovascular outcomes in patients with type 2 diabetes”. N Engl J Med 375.19 (2016): 1834-44.
- Zinman B., et al. “Empagliflozin, cardiovascular outcomes, and mortality in type 2 diabetes”. N Engl J Med373.22 (2015): 2117-28.
- Kernan WN., et al. “Pioglitazone after ischemic stroke or transient ischemic attack”. N Engl J Med 374.14 (2016): 1321-31.
- Dormandy JA., et al. “Secondary prevention of macrovascular events in patients with type 2 diabetes in the PROactive Study (PROspective pioglitAzone Clinical Trial In macroVascular Events): A randomised controlled trial”. The Lancet 366.9493 (2005): 1279-89.
- Einarson TR., et al. “Prevalence of cardiovascular disease in type 2 diabetes: a systematic literature review of scientific evidence from across the world in 2007–2017”. Cardiovasc Diabetol 17.1 (2018): 83.
- Malik MO., et al. “Ethnicity and risk of cardiovascular disease (CVD): 4.8 year follow-up of patients with type 2 diabetes living in Scotland”. Diabetologia 58.4 (2015): 716-25.
- Salinero-Fort MÁ., et al. “Cardiovascular and all-cause mortality in patients with type 2 diabetes mellitus in the MADIABETES Cohort Study: Association with chronic kidney disease”. J Diabetes Complications 30.2 (2016): 227-36.
- Carnethon MR., et al. “Diabetes and coronary heart disease as risk factors for mortality in older adults”. Am J Med 123.6 (2010): 556.e1–556.e9.
- Jackson CA., et al. “Area-based socioeconomic status, type 2 diabetes and cardiovascular mortality in Scotland”. Diabetologia 55.11 (2012): 2938-45.
- Mazza A., et al. “Serum uric acid shows a J-shaped trend with coronary mortality in non-insulin-dependent diabetic elderly people. The CArdiovascular STudy in the ELderly (CASTEL)”. Acta Diabetol 44.3 (2007): 99-105.
- Shestakova M. “Dynamics in prevalence of diabetes, diabetic complications and quality of diabetes care in Russian Federation in 2014–2015 by data of national diabetes register”. In: Conference: 52nd annual meeting of the European Association for the Study of Diabetes, EASD. (2016). p.309.
- Kucharska-Newton AM., et al. “Diabetes and the risk of sudden cardiac death, the Atherosclerosis Risk in Communities study”. Acta Diabetol 47.1 (2010): 161-8.
- Dey J. “SGLT2 inhibitor/DPP-4 inhibitor combination therapy–complementary mechanisms of action for management of type 2 diabetes mellitus”. Postgraduate medicine 129.4 (2017): 409-20.
- Mannucci E., et al. “Is glucose control important for prevention of cardiovascular disease in diabetes?” Diabetes Care 36(Supplement 2) (2013): S259-63.
- Fitchett D., et al. “Effects of empagliflozin on risk for cardiovascular death and heart failure hospitalization across the spectrum of heart failure risk in the EMPA-REG OUTCOME® trial”. Eur heart J 39.5 (2017): 363-70.
- Mudaliar S., et al. “Can a shift in fuel energetics explain the beneficial cardiorenal outcomes in the EMPA-REG OUTCOME study? A unifying hypothesis". Diabetes Care 39.7 (2016): 1115-22
- Cahill Jr GF. “Fuel metabolism in starvation”. Annu Rev Nutr 26 (2006): 1-22.
- Johansen OE., et al. “Cardiovascular safety with linagliptin in patients with type 2 diabetes mellitus: a pre-specified, prospective, and adjudicated meta-analysis of a phase 3 programme”. Cardiovasc Diabetol 11.1 (2012): 3.
- Rosenstock J., et al. “Cardiovascular safety of linagliptin in type 2 diabetes: a comprehensive patient-level pooled analysis of prospectively adjudicated cardiovascular events”. Cardiovasc Diabetol 14.1 (2015): 57.
- Rosenstock J., et al. “Effect of Linagliptin vs Placebo on Major Cardiovascular Events in Adults with Type 2 Diabetes and High Cardiovascular and Renal Risk: The CARMELINA Randomized Clinical Trial”. JAMA. (2018) Nov 9.
- Scirica BM., et al. “SAVOR-TIMI 53 Steering Committee and Investigators. Saxagliptin and cardiovascular outcomes in patients with type 2 diabetes mellitus”. N Engl J Med 369.14 (2013): 1317-1326.
- White WB., et al. “Alogliptin after acute coronary syndrome in patients with type 2 diabetes”. N Engl J Med 369.14 (2013): 1327-1335.
- Green JB., et al. “Effect of sitagliptin on cardiovascular outcomes in type 2 diabetes”. N Engl J Med 373.3 (2015): 232-242.
- Ansar S., et al. “Postprandial hyperlipidemia, endothelial dysfunction and cardiovascular risk: focus on incretins”. Cardiovascular Diabetol 10.1 (2011): 61.
- Fadini GP and Avogaro A. “Cardiovascular effects of DPP-4 inhibition: beyond GLP-1”. Vascul Pharmacol. 55(1-3) (2011): 10-16.
- Brownlee M. “The pathobiology of diabetic complications: a unifying mechanism”. Diabetes 54.6 (2005): 1615-25.
- Lewin A., et al. “Initial combination of empagliflozin and linagliptin in subjects with type 2 diabetes”. Diabetes Care 38.3 (2015): 394-402.
- DeFronzo RA., et al. “Combination of empagliflozin and linagliptin as second-line therapy in subjects with type 2 diabetes inadequately controlled on metformin”. Diabetes Care 38.3 (2015): 384-93.
- Tinahones FJ., et al. “Linagliptin as add‐on to empagliflozin and metformin in patients with type 2 diabetes: Two 24‐week randomized, double‐blind, double‐dummy, parallel‐group trials”. Diabetes Obes Metab 19.2 (2017): 266-74.
- Søfteland E., et al. “Empagliflozin as add-on therapy in patients with type 2 diabetes inadequately controlled with linagliptin and metformin: a 24-week randomized, double-blind, parallel-group trial”. Diabetes Care 40.2 (2017): 201-9.
- Sharma MD. “Potential for combination of dipeptidyl peptidase‐4 inhibitors and sodium‐glucose co‐transporter‐2 inhibitors for the treatment of type 2 diabetes”. Diabetes Obes Meta 17.7 (2015): 616-21.
Citation:
Sneha Thakur., et al. “Beyond Glycemic Control: Cardiovascular Benefits with Empagliflozin and Linagliptin Combination.” Archives of Endocrinology and Diabetes Care 2.2 (2019): 187-193.
Copyright: © 2019 Sneha Thakur., et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.































 Scientia Ricerca is licensed and content of this site is available under a Creative Commons Attribution 4.0 International License.
Scientia Ricerca is licensed and content of this site is available under a Creative Commons Attribution 4.0 International License.